Rotator Cuff Tear Arthritis
Rotator Cuff Tear Arthritis
Rotator cuff tear arthritis is a particular type of arthritis that afflicts the glenohumeral joint (ball and socket joint) of the shoulder. As the name suggests, this particular type of arthritis arises gradually due to the deterioration of the rotator cuff over time. The rotator cuff are the 4 muscles of the shoulder that arise from the scapula (shoulder blade bone) and attach to the humeral head (ball of the shoulder joint).
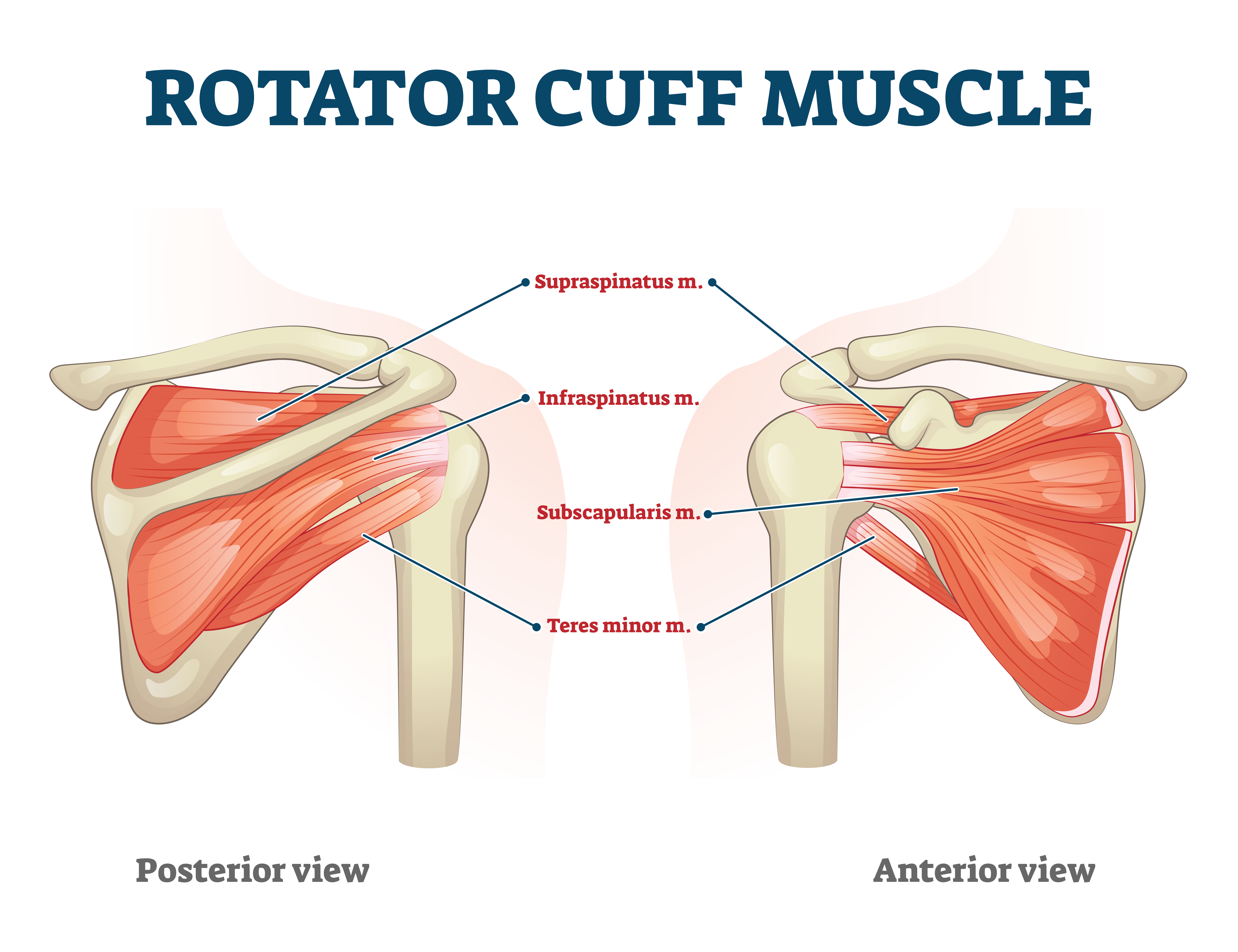
Functions of the 4 Rotator Cuff Muscles
The first function is to help place the arm in space
The shoulder joint is naturally a joint that has enormous degrees of freedom in motion so that we can reach in a maximum range of motion around our body. This allows us to put our hand in space so that we can reach objects away from us in all sorts of directions. The rotator cuff muscles work together to help us precisely put our hand in any space around the range of motion the shoulder allows.
The second function of the rotator cuff is to keep the ball centered on the socket when we reach away from our bodies, especially overhead
The rotator cuff pushes the ball down into the center of the socket to counteract the very large force that the very large deltoid muscles create to generate power in the shoulder. In effect, as the deltoid pulls the ball of the shoulder up towards the top of the socket, the rotator cuff pushes the ball down to the center. This balance allows for the smooth effortless motion of the shoulder we enjoy.
When the rotator cuff begins to tear and/or weaken over time, the balance between the rotator cuff and the deltoid muscle begins to fail. The deltoid muscle overpowers the dysfunctional rotator cuff and lifts the ball towards the top of the socket. This abnormal motion gradually erodes the cartilage surfaces of the ball (humeral head) and the socket (glenoid). As the rotator cuff tears more, the abnormal motion and position of the glenohumeral joint is magnified. As a result, the arthritis changes accelerate.
With severe rotator cuff tears and dysfunction, the humeral head establishes a new resting position that is high against the glenoid. In severe cases, the humeral head can begin to articulate with the undersurface of the acromion. The humeral head and glenoid can develop secondary deformities.
Patients who develop rotator cuff tear arthritis gradually experience progressive loss of overhead motion, progressive overhead weakness, and feel a sense of grinding in their affected shoulder.
Eventually, if enough of the rotator cuff has deteriorated and enough positional deformity has developed, patients can experience a condition known as pseudoparalysis. As the name suggests, pseudoparalysis is a condition in which the shoulder dysfunction mimics that of a paralyzed shoulder. Patients with pseudoparalysis cannot raise their affected shoulder with the use of the shoulder muscles. They are unable to use the deltoid muscles to elevate overhead or abduct the arm.
Treatment for Rotator Cuff Tear Arthritis
Treatment for rotator cuff tear arthritis is catered to the individual patient’s goals, expectations, and physical requirements.
Pain control and therapy
Conservative treatment for rotator cuff tear arthritis include modalities for pain control such as the use of anti-inflammatory medications and steroid injections when necessary. For functional overhead use recovery in patients with early rotator cuff tear arthritis findings, a structured physical therapy program and home exercises can strengthen the anterior and posterior rotator cuffs to better counterbalance the superior pull of the deltoid muscles. If successful, therapy can restore better overhead function in the affected shoulder. For therapy to succeed, adequate rotator cuff must be intact such that it can be strengthened. In general, for therapy to succeed, the anterior (subscapularis) and posterior (teres minor and infraspinatus) rotator cuff muscles must be intact as these form what is known as the A-P force couple of the shoulder.
If conservative measures fail to relieve pain and/or the patient is unable to successfully recover overhead use with therapy, surgical intervention is considered.
Surgical solution
Surgery for rotator cuff tear arthritis is in the form of a special type of shoulder replacement known as a reverse total shoulder replacement (arthroplasty). Reverse total shoulder arthroplasty has been done in the United States since it was FDA approved in 2004. It has been reliably done in Asia, Europe, and Australia since the early 1990s.
As the name suggests, reverse total shoulder arthroplasty is a total joint replacement in which the ball and socket components are “reversed” in their configuration when compared to a normal shoulder joint. In other words, the ball component (the glenosphere) is placed onto the native socket (the glenoid); and the socket component (the cup) is placed onto the native proximal humerus (the ball side).
A reverse total shoulder arthroplasty by design bypasses the deficient and dysfunctional rotator cuff and mechanically “re-centers” the glenohumeral joint. In doing so, the reverse replacement utilizes the deltoid muscles to effectively elevate and abduct the arm into the overhead positions.
One caveat of reverse shoulder replacements is that it cannot overcome a deficiency of the posterior rotator cuff muscles. The posterior rotator cuff muscles are responsible for the shoulder’s ability to externally rotate the arm. Without these muscles, we cannot put our hands onto the backs of our heads.
In a rotator cuff tear arthritis shoulder with a deficient posterior rotator cuff, it is important to create a posterior rotator cuff when doing a reverse shoulder replacement. If a posterior rotator cuff muscle is not “created”, patients will experience a functional deficit known as a “hornblower’s sign” when they elevate their arm overhead. This inability to externally rotate the arm makes it difficult for patients to reach the backs of their heads and use utensils such as spoons to eat, brush their teeth, or comb their hair.
If the posterior rotator cuff is deficient, an additional procedure called a muscle transfer is performed to create a new posterior rotator cuff. This procedure is done at the same time as the reverse shoulder replacement. Generally, a muscle called the latissimus dorsi is transferred to the posterior shoulder to become the “new” external rotator of the shoulder. This muscle transfer can be done through the same incision as the one for the reverse total shoulder replacement and has shown to be very successful at restoring the ability to externally rotate the shoulder.
Reverse total shoulder replacement has become a very reliable procedure in the hands of fellowship trained shoulder surgeons to help patients who suffer from dysfunction and pain due to rotator cuff tear arthritis. The accepted longevity of reverse shoulder replacements is currently projected to be anywhere from 15-20 years. The average recovery time to functional activities of daily living use is anywhere from 12-16 weeks after surgery. Maximum recovery of motion and strength can take up to 6-8 months for most patients.
As with any surgery, there are potential pitfalls and complications that can arise. In general, the risks associated with reverse total shoulder arthroplasty range in the 1-2 % range for most common complications. The percentages are less for less common complications.
If a patient is healthy, has good home support for after surgery care, and their insurance permits, reverse total shoulder arthroplasty can be safely done as an outpatient procedure. The surgical time for reverse total shoulder arthroplasty is generally anywhere from 45 minutes straightforward cases to 2 hours for complex deformity cases.
Contact Boise’s Leading Shoulder Surgeon Today
Whether you’ve been diagnosed with rotator cuff tear arthritis or you’ve been living with chronic unexplained shoulder dysfunction and pain for too long, our shoulder fellowship trained surgeon can help.

